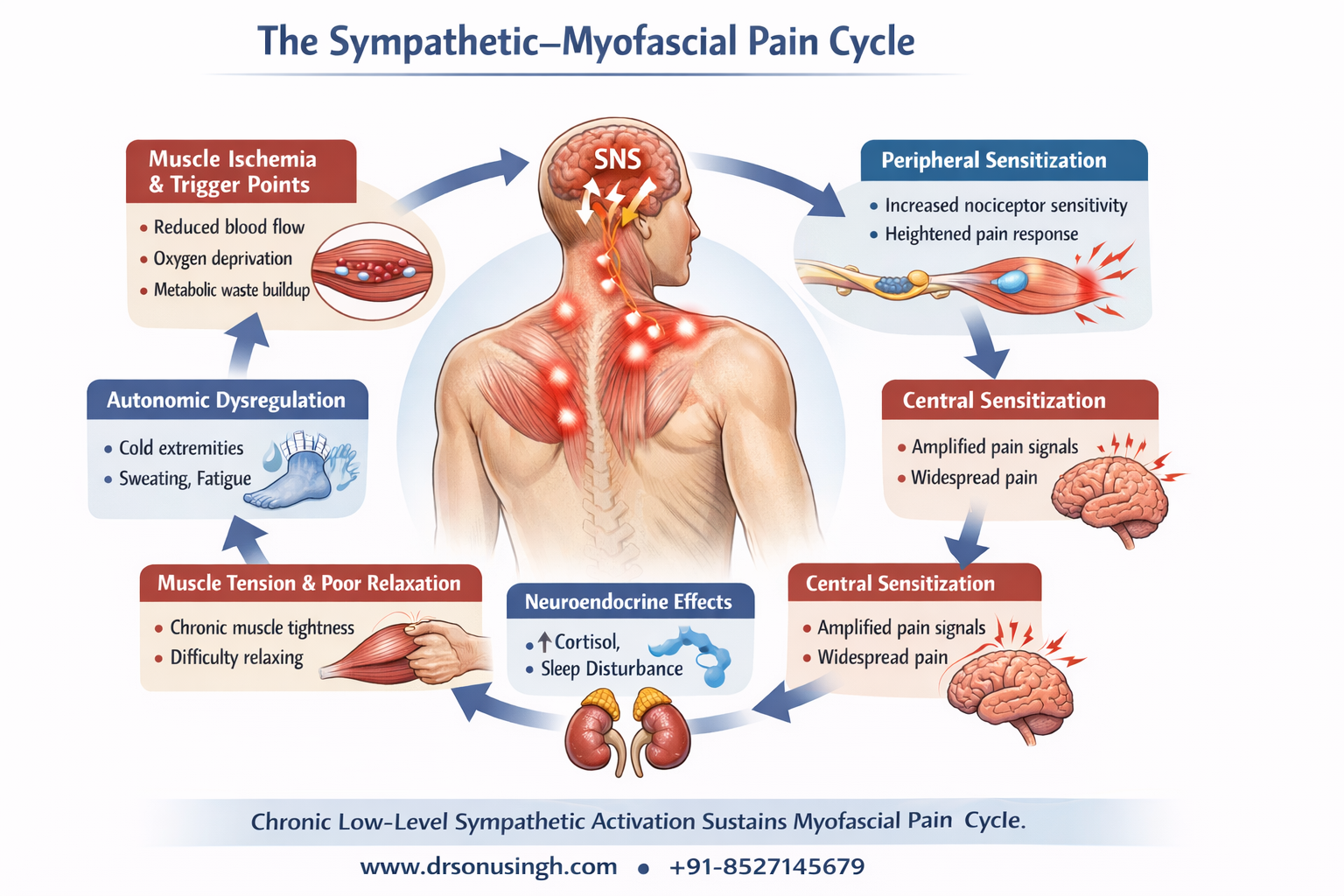
Chronic myofascial pain syndrome (MPS) is often associated with persistent low-level activation of the sympathetic nervous system (SNS). Instead of short bursts of “fight-or-flight” activation, the body remains in a mild but continuous sympathetic state, which can produce multiple physiological and clinical consequences.
1. Sustained Muscle Ischemia and Energy Crisis
Persistent sympathetic tone causes vasoconstriction in skeletal muscle microcirculation.
Effects
-
Reduced local blood flow
-
Decreased oxygen delivery
-
Accumulation of metabolic waste (lactate, bradykinin, substance P)
Clinical result
-
Formation and persistence of myofascial trigger points
-
Local muscle stiffness and tenderness
-
Increased pain sensitivity
This phenomenon is sometimes called the “energy crisis hypothesis” of myofascial pain.
2. Peripheral Sensitization
Chronic sympathetic activation increases the sensitivity of nociceptors in muscle.
Mechanisms include:
-
Increased release of inflammatory mediators
-
Lowered pain threshold of sensory fibers
-
Upregulation of adrenergic receptors on nociceptive fibers
Outcome
-
Non-painful stimuli may become painful (allodynia)
-
Pain intensity increases (hyperalgesia)
3. Central Sensitization
Long-standing nociceptive input from trigger points can alter pain processing in the spinal cord and brain.
Effects include:
-
Amplification of pain signals
-
Expansion of receptive fields
-
Persistent pain even after the original tissue stimulus decreases
This explains why chronic myofascial pain can evolve into widespread pain syndromes.
4. Autonomic Dysregulation
Continuous sympathetic tone may produce several autonomic symptoms:
-
Cold extremities
-
Increased sweating
-
Altered skin blood flow
-
Sleep disturbance
-
Increased fatigue
These symptoms are frequently reported in patients with chronic neck and shoulder myofascial pain.
5. Impaired Muscle Relaxation
Sympathetic overactivity increases gamma motor neuron activity, which increases muscle spindle sensitivity.
Consequences:
-
Persistent muscle contraction
-
Increased muscle tone
-
Reduced muscle relaxation during rest
This creates a pain–spasm–pain cycle.
6. Neuroendocrine Effects
Chronic sympathetic activation also stimulates the hypothalamic-pituitary-adrenal (HPA) axis.
Possible systemic effects:
-
Elevated cortisol levels
-
Sleep disturbances
-
Fatigue
-
Reduced recovery capacity
7. Psychological and Cognitive Effects
Long-term sympathetic arousal contributes to:
-
Anxiety
-
Reduced stress tolerance
-
Difficulty concentrating
-
Poor sleep quality
These factors further increase pain perception.
Clinical Implication in Myofascial Pain
Management strategies should aim to break the sympathetic overactivity cycle, including:
-
Myofascial trigger point therapy
-
Postural and biomechanical correction
-
Stretching and rehabilitation exercises
-
Relaxation and breathing techniques
-
Adequate sleep and stress control
-
Sometimes medications that modulate autonomic tone
Addressing both musculoskeletal and autonomic components is crucial for long-term recovery.
Chronic myofascial pain is not purely a local muscle disorder. Persistent low-level sympathetic activation contributes to ischemia, trigger point formation, peripheral and central sensitization, and autonomic dysfunction, perpetuating the pain cycle.